How Do You Manage Urinary Issues?
Most urinary issues—like leakage, urgency, or incomplete emptying—can be significantly improved with a combination of pelvic floor physical therapy, bladder training, lifestyle changes, and medical guidance when needed. Maintaining a healthy weight through regular exercise and healthy eating can help reduce the risk of urinary issues. The key is identifying the root cause (muscle weakness, nerve dysfunction, hormonal shifts, or prostate issues) and following a personalized treatment plan. It is important to consult a healthcare provider to develop a management strategy tailored to your needs and to address any underlying health problems.
For many adults aged 21–48, conservative care such as pelvic floor therapy is the first and most effective step.
Urinary problems are more common than most people realize—and they don’t only affect older adults. In my clinical practice as a pelvic health physical therapist, I regularly treat men and women in their 20s, 30s, and 40s dealing with:
- Sudden urgency
- Leakage during workouts
- Postpartum bladder control changes
- Frequent nighttime urination
- Difficulty fully emptying the bladder
- Bladder control problems that may cause some people to leak urine or limit their activities in fear of not making it to a bathroom in time
According to the National Association for Continence, over 25 million Americans experience some form of urinary incontinence. The Centers for Disease Control and Prevention reports that urinary incontinence affects nearly 1 in 3 women at some point in their lives. Bladder control problems can significantly impact daily life, especially if you avoid activities because you are worried about not reaching the bathroom in time.
The good news? Most urinary dysfunction is treatable—and often reversible—with the right approach.
What Are Urinary Issues?
Urinary issues refer to dysfunction involving the bladder, urethra, nerves, or pelvic floor muscles that interfere with normal urination.
Common symptoms include:
- Urine leakage (incontinence)
- Frequent urination (more than 8 times daily)
- Sudden, intense urgency or urge to urinate
- Strong urge or intense urge to pass urine
- Painful urination
- Weak urine stream
- Feeling unable to fully empty the bladder
- Blood in the urine
- Cloudy or foul-smelling urine
- Waking up more than once each night to pass urine (nocturia)
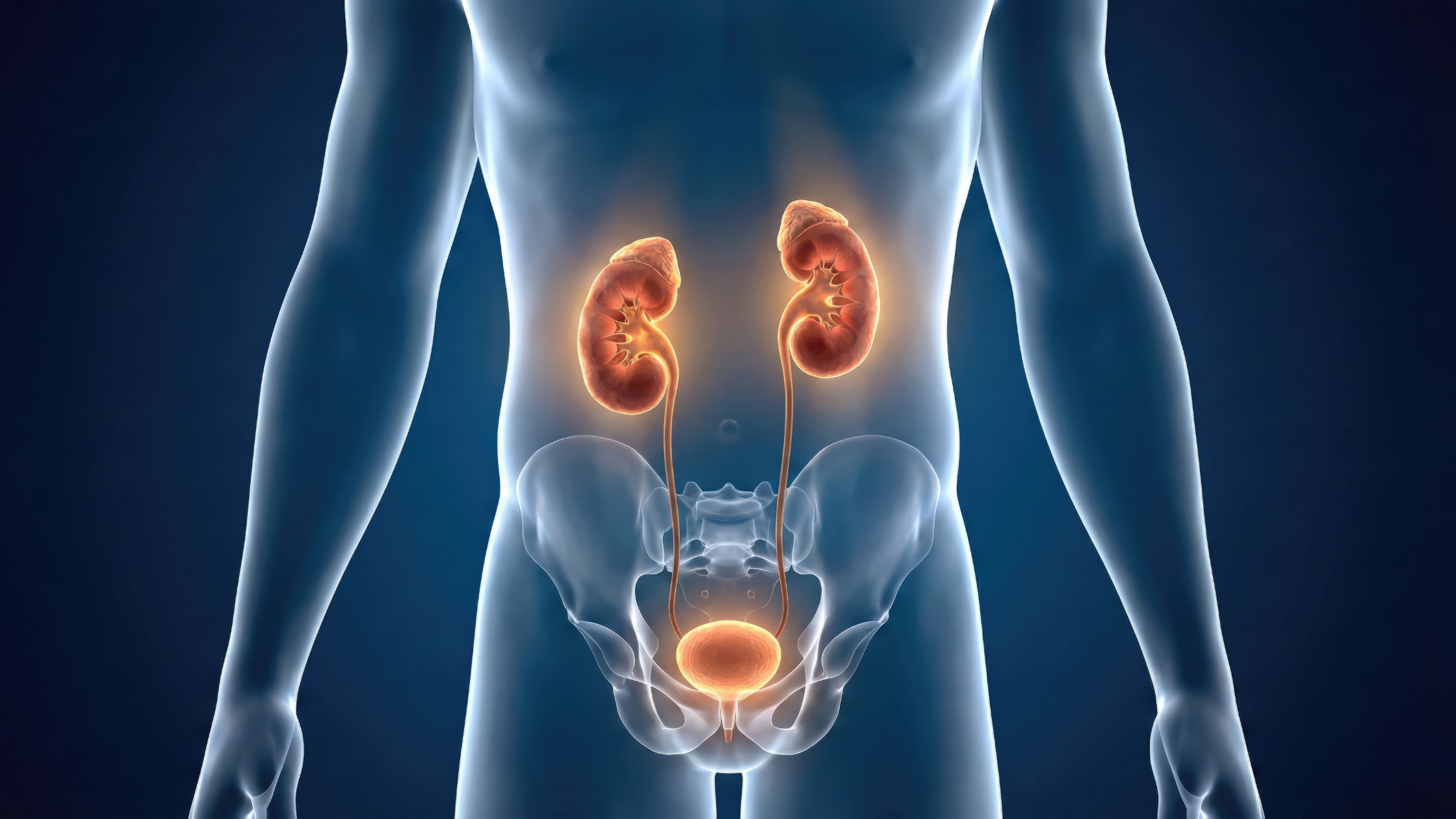
The urinary system includes the kidneys, bladder, ureters, and urethra. These organs work together to carry urine out of the body.
The bladder itself is a muscular organ about the size of a grapefruit when full. It relies heavily on coordination between:
- The detrusor muscle (bladder muscle)
- The urethral sphincter
- The pelvic floor muscles
- The nervous system
Nerves and muscles, including the sphincter muscles, coordinate through nerve signals to control bladder function. Proper communication between these components is essential for normal urination, and disruptions can lead to urinary issues.
A bladder diary and pad test are useful tools for tracking symptoms and diagnosing urinary issues.
When this system falls out of sync, symptoms begin.
Types of Urinary Incontinence (And Why It Matters)
Not all bladder leaks are the same. Bladder control problems and bladder control issues can affect anyone, but they are more common in certain groups and at certain times in life, such as during pregnancy, after childbirth, menopause, or with prostate problems in men. Understanding the type helps determine the correct treatment.
1. Stress Incontinence
Leakage triggered by coughing, laughing, jumping, or lifting. Common in postpartum women and athletes.
Cause: Stress incontinence occurs when weakened pelvic floor muscles, often due to childbirth or aging, make it hard for the bladder to hold urine. The primary symptom is leaking urine before you can make it to the bathroom or during activities like sneezing, coughing, laughing, or exercising.
2. Urge Incontinence
Sudden, overwhelming need to urinate, often described as a strong urge or intense urge, followed by leakage. This is characteristic of urge incontinence, where the sudden, intense urge to urinate is difficult to control and may result in involuntary urine leakage.
Often linked to overactive bladder (OAB).
Cause: Involuntary bladder contractions.
Dietary bladder irritants can also increase urinary frequency and urgency.
3. Overflow Incontinence
Dribbling caused by incomplete bladder emptying.
Cause: Obstruction (e.g., enlarged prostate) or nerve dysfunction. Overflow incontinence can be associated with urinary retention, which is the inability to completely empty the bladder. Urinary retention is commonly caused by physical blockages or nerve damage.
4. Functional Incontinence
Physical or mobility barriers prevent timely bathroom access.
Why Are Urinary Issues Happening at 21–48 Years Old?
Many younger adults are surprised when bladder symptoms appear. Common triggers include:
- Drinking caffeine or alcohol late in the day
- High fluid intake before bed
- Stress or anxiety
- Certain medications
Underlying health issues can also contribute to urinary symptoms. A sudden increase in urination that can’t be explained, especially at night, may indicate a bladder problem or diabetes.
For Women
- Pregnancy and childbirth
- Hormonal shifts
- High-impact exercise
- Chronic constipation
Pelvic floor exercises during and after pregnancy can help prevent urinary incontinence by strengthening the pelvic muscles.
For Men
- Prostate inflammation
Prostate inflammation, or prostatitis, can lead to urinary issues such as pain, urgency, and frequent urination. Benign prostatic hyperplasia (BPH) is another common, non-cancerous enlargement of the prostate gland that can cause urinary difficulties, such as trouble starting urination or incomplete bladder emptying, especially as men age.
- Chronic straining
- Post-surgical changes
- Pelvic floor tension
For Both
- Stress and anxiety
- Caffeine overload
- Sedentary lifestyle
- Heavy lifting without core coordination. Certain physical activities, such as high-impact exercise, can also trigger stress incontinence by increasing pressure on the bladder.
Research published in the Journal of Women’s Health Physical Therapy shows pelvic floor muscle training improves stress incontinence symptoms by up to 70% in appropriately selected patients.
How Pelvic Floor Physical Therapy Helps Urinary Incontinence
Pelvic floor therapy is often the most underutilized yet highly effective treatment for urinary dysfunction.
As a Doctor of Physical Therapy specializing in pelvic health, I assess:
- Muscle strength
- Coordination
- Endurance
- Relaxation ability
- Breathing mechanics
- Core and hip function
- Bladder muscles and the coordination of nerves and muscles that control bladder function
Keeping a bladder diary is also recommended to track urination patterns, symptoms, and progress, which can help identify urinary issues and guide treatment.
Treatment May Include:
- Targeted Kegel progressions (not generic instructions)
- Biofeedback training
- Electrical stimulation (if appropriate)
- Manual therapy for tight muscles
- Bladder retraining protocols
- Behavioral strategies
A pad test may also be used during assessment to objectively measure urine leakage, involving a specially treated pad that changes color upon urine leakage.
A 2018 systematic review published in Cochrane Database of Systematic Reviews found pelvic floor muscle training significantly improves or cures stress urinary incontinence compared to no treatment.
Why This Matters
Many people try random Kegels they found online. But doing them incorrectly—or when muscles are actually tight—can worsen symptoms.
Professional guidance ensures:
- Correct diagnosis
- Proper muscle activation
- Customized progression
If you’re in New York City, you can schedule an evaluation at Pelvis NYC for personalized care from pelvic health specialists.
Bladder Training: How to Retrain Urgency
If you feel like you’re constantly running to the bathroom, bladder training can help.
Step-by-Step Approach
- Track urination patterns for 3 days.
- Set scheduled voiding intervals.
- Gradually increase time between bathroom trips.
- Use urge-suppression breathing techniques.
Many patients improve urgency within 4–6 weeks.
Hydration & Diet: What Actually Helps?
Drinking habits, such as alcohol and caffeine intake, can significantly affect bladder health. Consuming alcohol and caffeine can cause the body to produce more urine, which may irritate the bladder and increase urination frequency. Hydration is important for bladder health—too little fluid can irritate the bladder, while too much can increase frequency. Dietary adjustments for managing urinary issues include limiting bladder irritants like caffeine, alcohol, and spicy foods. Cutting down on alcohol and caffeine can help manage urinary health.
Bladder irritants are often overlooked contributors.
Reduce or Eliminate:
- Caffeine
- Alcohol
- Artificial sweeteners
- Carbonated drinks
- Highly acidic foods
Improve With:
- 6–8 glasses of water spaced evenly
- Increased fiber (25–30g daily)
- Anti-inflammatory foods
Constipation increases pelvic floor pressure and can worsen incontinence.
Painful Urination: When to See a Doctor

Burning or pain during urination may indicate:
- Urinary tract infection (UTI)
- Interstitial cystitis
- Pelvic floor tension
- Hormonal changes
- Prostate inflammation
The Mayo Clinic advises seeking medical evaluation if painful urination is persistent, accompanied by fever, or includes blood in urine.
Always rule out infection first. If labs are clear, pelvic floor dysfunction may be the hidden cause.
Lifestyle Adjustments That Make a Big Difference
Here are practical, real-world changes I recommend to patients:
Maintain a healthy weight through regular physical activities, as this can help reduce the risk of urinary issues.
Limit caffeine and alcohol, as these can irritate the bladder.
Try to drink less fluid before bedtime to help reduce nighttime urination.
Schedule bathroom visits every 2-4 hours, even if you don’t feel the urge.
Practice pelvic floor exercises (Kegels) to strengthen the muscles that control urination.
1. Stop “Just in Case” Bathroom Trips
Frequent preventive urination shrinks bladder capacity.
2. Coordinate Breathing with Movement
Exhale during lifting to reduce pressure on the pelvic floor.
3. Strengthen Your Hips and Core
Pelvic stability improves bladder control.
4. Manage Stress
Chronic tension affects pelvic floor relaxation.
Medical Treatment Options (When Needed)
If conservative therapy isn’t enough:
- Anticholinergic medications
- Beta-3 agonists
- Neuromodulation therapy
- Botox injections
- Surgery: Surgical treatment for stress incontinence may involve a sling procedure to reduce pressure on the bladder.
Physical therapy is often recommended before surgical intervention.
Real Case Example
A 34-year-old fitness instructor came to our clinic with stress incontinence during jump training. She assumed it was “normal after childbirth.”
After 8 sessions of pelvic floor therapy focused on coordination (not just strength), she returned to full workouts without leakage.
Bladder dysfunction is common—but not normal.
Frequently Asked Questions (FAQ)
What is the fastest way to stop urinary leakage?
The fastest improvement typically comes from guided pelvic floor physical therapy combined with bladder habit changes.
Can urinary incontinence go away on its own?
Mild cases sometimes improve, but most benefit from structured treatment.
How long does pelvic floor therapy take?
Most patients notice improvement within 4–8 weeks.
Are Kegels enough to fix bladder leaks?
Not always. Incorrect technique or underlying tension can worsen symptoms.
When should I see a specialist?
If symptoms last more than 2–4 weeks, interfere with exercise, sleep, or daily life, seek evaluation.
Take Control of Your Bladder Health
Urinary issues can feel isolating—but they are highly treatable. Whether you’re dealing with leaks during workouts, postpartum changes, or sudden urgency at work, help is available.
At Pelvis NYC, we specialize in evidence-based pelvic floor physical therapy for men and women.
👉 Schedule your consultation today at www.pelvis.nyc and take the first step toward lasting bladder control.

